GT Investigates: US failure in epidemic control drives burnout among medics in two-year COVID battle
Sacrifices in vain
Editor's note:
Western countries, one by one, have scrapped their COVID-19 restrictions and purported to be ready to "return to normalcy." Yet, as the coronavirus continues to mutate, from the deadly Delta variant to the more contagious, milder Omicron variant, what can such a rush to reopen really bring to the West in the post-pandemic era? Analyzing data and talking to epidemiologists, the Global Times conducted a series of investigations into what consequences the vulnerable groups, including the elderly, the minorities and children, would have to bear when their countries ease COVID-19 restrictions, and what impact such moves would wreak on the medical systems of these countries. This is the third installment, looking into the shocking impact of the US' easing of anti-epidemic restrictions on their frontline heroes - healthcare workers.
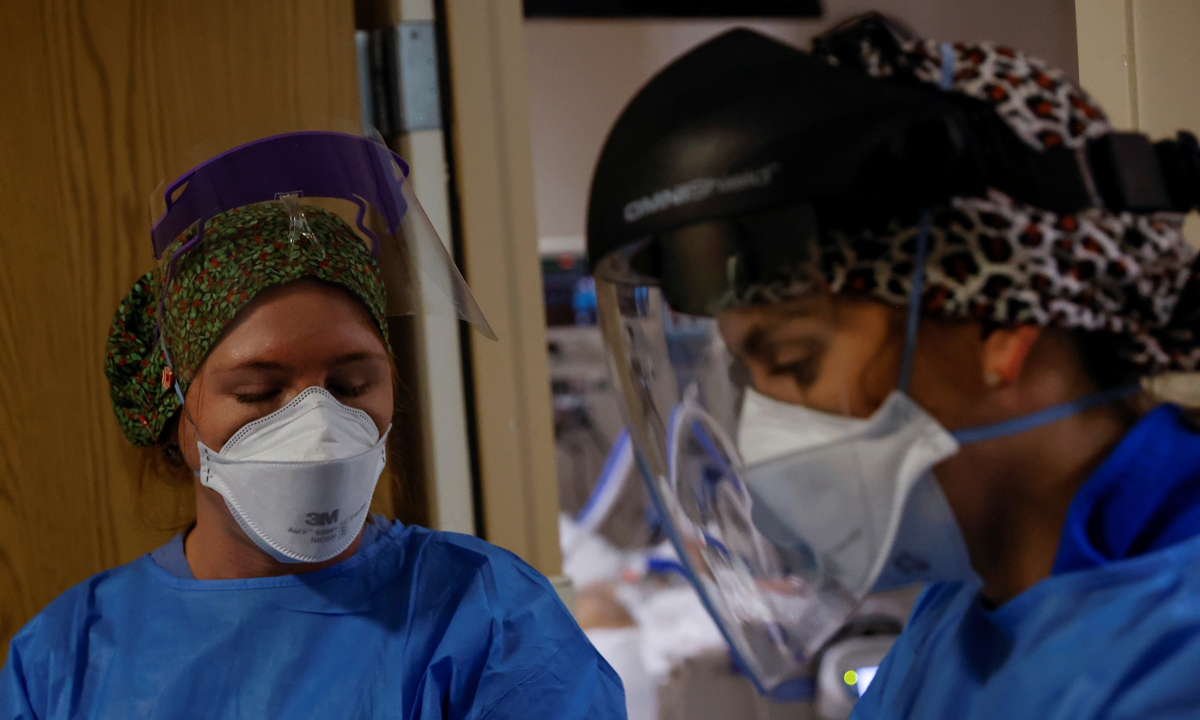
While US President Joe Biden mourned 1 million American deaths from COVID-19 on Thursday, the US has been facing a crisis of burnout among its healthcare workers.
Mendy, a Virginia-based healthcare worker - only giving her first name - who has been working in the sector for 22 years, has to work long hours and she said the COVID-19 pandemic has "wrecked havoc in the medical field."
When she talked with the Global Times via social media, she said that on many days, medical staff work without proper personal protective equipment, and they have to work very long hours - 12 to 16 hours a day and sometimes seven days a week. "We are always short-staffed, we miss lunch and go for hours without a chance to use the bathroom," she said.
American healthcare workers who had been fighting the pandemic at the frontline have also become one of the most vulnerable groups along with the elderly population. About 3,600 healthcare workers died in 2020, NBC reported on May 6, citing a Kaiser Health News investigation.
The pandemic may have a long-lasting impact, as some healthcare workers have described it as "long COVID" for healthcare professionals.
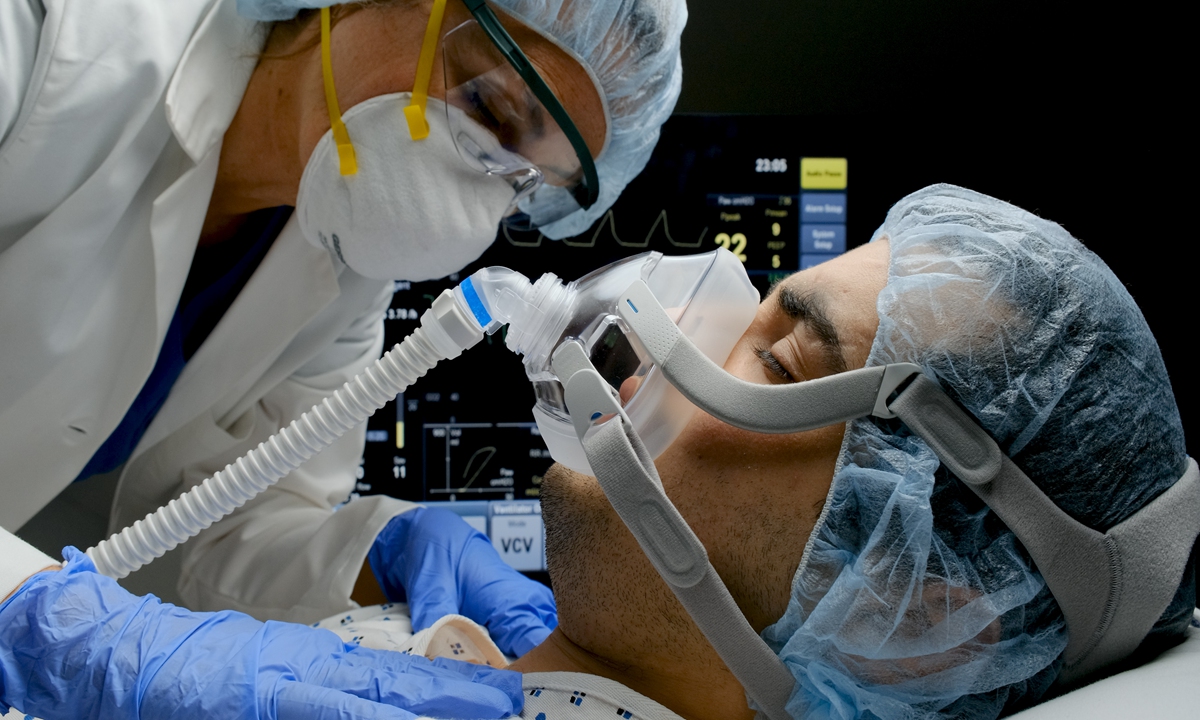
Burden on American medics
With Omicron infections showing milder symptoms, some experts have considered "coexisting with the virus." Some US industry lobbying groups also urged relaxation of the mask mandate in public places like on the flights. But the new variant is not that mild, even though the hospitalization rate trended downward in early 2022. Omicron set records for COVID infections in the US, causing a sharp increase in hospitalizations among youngsters.
And the average number of hospitalized patients with confirmed COVID-19 is up 44 percent from a mid-April low, the Wall Street Journal reported on May 9, citing federal data. Some places that have avoided the worst of the pandemic, including Puerto Rico and Northern New England states, are coping with elevated cases and hospitalizations as the latest highly contagious iterations of the virus circulate, the WSJ said.
"Frontline medical workers are exhausted and burned out," Eric Ding from the Federation of American Scientists told the Global Times. He noted that he hopes that more care will be given to airborne risk in buildings via ventilation and air disinfection.
In addition to the long working hours and growing stress, the medical workers' pay rates do not reflect the rising inflation in the country, Mendy told the Global Times. As she worked at a long-term care facility offering medical-surgical nursing, a COVID unit and an assisted living facility, she said she had seen many of her coworkers quit, change their careers or retire early.
"It's because the job had become too physically and mentally draining," she said.
As Omicron peaked, the US healthcare system has been "left broken beyond repair," the Guardian said in an article in February. An emergency physician in the San Francisco Bay Area, who recently polled a group of doctors on an overnight shift about their jobs, said that the ripple effects of the virus, such as its impact on patients needing care for other issues, continue to test the limits of the US healthcare system and its providers despite an overall decreased hospitalization rate.
A recent survey from Elsevier Health - a provider of information solutions for science, health and technology professionals - showed that up to 47 percent of the US healthcare workers plan to leave their positions by 2025. And experts at the Association of American Medical Colleges (AAMC) shared a similar estimation, saying that the US will come up short on physicians within just a dozen years, by somewhere between 37,800 and 124,000 doctors.
By one calculation, that is the number of US physicians in direct care who left the workforce between the start of 2019 and the fall of 2021, even before the Omicron wave slammed intensive care units and left too many doctors feeling desperate amid a "pandemic of mistrust," AAMC said on May 4.

A different strategy
American healthcare workers have been facing tremendous stress because the overall anti-epidemic strategy in the US is a mitigation policy, rather than an elimination policy, to curb the peak of the transmission, but the hospitalization rate for the past two years remained high, Chen Xi, an associated professor of public health at Yale University, told the Global Times.
"Although the hospitalization rates have recently dropped, the overall rates over the past two years remain very high, which means the medical staff have been working under stress and have been exposed to the risk of getting infected, which is why many of them have left their positions," Chen said.
In the initial phases of the COVID-19 pandemic, many US hospitals could not provide an adequate supply of beds to meet the demand, and the burgeoning Omicron variant is already overwhelming US hospitals because of high rates of hospitalization, Washington DC-based healthcare publication Health Affairs said in an article in February. When compared globally, the US has relatively low number of hospital beds, with only 2.8 beds per thousand people compared to 8.0 beds per thousand people in Germany, according to the publication.
According to the Chinese health authorities, China's number of hospital beds per thousand people increased from 6.30 in 2019 to 6.46 in 2020, but this is still behind some developed countries and regions.
Liang Wannian, head of the COVID-19 response expert panel under the National Health Commission (NHC), told a press conference on April 29 that as China has an unbalanced regional spread of population and a lack of medical resources in some areas, a strategy of "coexisting with the virus" would put too much pressure on the country's medical resources, posing a serious threat to those with underlying diseases, elderly groups, children and pregnant women.
Chinese health authorities, in accordance with the country's dynamic zero-COVID strategy, recently updated the COVID-19 treatment playbook to reduce the burden on Chinese medical workers. For example, mild cases are isolated rather than being taken to hospital, which can avoid hospitals becoming overwhelmed.
As the virus variant continues spreading in the US, the hospitalization rate will increase, highlighting the shortage of medical staff, Chen noted.
"In the next phase, the medical workers in the US will still be under a lot of stress," he said.
Western countries, one by one, have scrapped their COVID-19 restrictions and purported to be ready to "return to normalcy." Yet, as the coronavirus continues to mutate, from the deadly Delta variant to the more contagious, milder Omicron variant, what can such a rush to reopen really bring to the West in the post-pandemic era? Analyzing data and talking to epidemiologists, the Global Times conducted a series of investigations into what consequences the vulnerable groups, including the elderly, the minorities and children, would have to bear when their countries ease COVID-19 restrictions, and what impact such moves would wreak on the medical systems of these countries. This is the third installment, looking into the shocking impact of the US' easing of anti-epidemic restrictions on their frontline heroes - healthcare workers.

Medical staff treat a COVID-19 patient in the ICU at a hospital in Mission Viejo, California, US, on January 25, 2022. Photo: IC
While US President Joe Biden mourned 1 million American deaths from COVID-19 on Thursday, the US has been facing a crisis of burnout among its healthcare workers.
Mendy, a Virginia-based healthcare worker - only giving her first name - who has been working in the sector for 22 years, has to work long hours and she said the COVID-19 pandemic has "wrecked havoc in the medical field."
When she talked with the Global Times via social media, she said that on many days, medical staff work without proper personal protective equipment, and they have to work very long hours - 12 to 16 hours a day and sometimes seven days a week. "We are always short-staffed, we miss lunch and go for hours without a chance to use the bathroom," she said.
American healthcare workers who had been fighting the pandemic at the frontline have also become one of the most vulnerable groups along with the elderly population. About 3,600 healthcare workers died in 2020, NBC reported on May 6, citing a Kaiser Health News investigation.
The pandemic may have a long-lasting impact, as some healthcare workers have described it as "long COVID" for healthcare professionals.

Photo: VCG
Burden on American medics
With Omicron infections showing milder symptoms, some experts have considered "coexisting with the virus." Some US industry lobbying groups also urged relaxation of the mask mandate in public places like on the flights. But the new variant is not that mild, even though the hospitalization rate trended downward in early 2022. Omicron set records for COVID infections in the US, causing a sharp increase in hospitalizations among youngsters.
And the average number of hospitalized patients with confirmed COVID-19 is up 44 percent from a mid-April low, the Wall Street Journal reported on May 9, citing federal data. Some places that have avoided the worst of the pandemic, including Puerto Rico and Northern New England states, are coping with elevated cases and hospitalizations as the latest highly contagious iterations of the virus circulate, the WSJ said.
"Frontline medical workers are exhausted and burned out," Eric Ding from the Federation of American Scientists told the Global Times. He noted that he hopes that more care will be given to airborne risk in buildings via ventilation and air disinfection.
In addition to the long working hours and growing stress, the medical workers' pay rates do not reflect the rising inflation in the country, Mendy told the Global Times. As she worked at a long-term care facility offering medical-surgical nursing, a COVID unit and an assisted living facility, she said she had seen many of her coworkers quit, change their careers or retire early.
"It's because the job had become too physically and mentally draining," she said.
As Omicron peaked, the US healthcare system has been "left broken beyond repair," the Guardian said in an article in February. An emergency physician in the San Francisco Bay Area, who recently polled a group of doctors on an overnight shift about their jobs, said that the ripple effects of the virus, such as its impact on patients needing care for other issues, continue to test the limits of the US healthcare system and its providers despite an overall decreased hospitalization rate.
A recent survey from Elsevier Health - a provider of information solutions for science, health and technology professionals - showed that up to 47 percent of the US healthcare workers plan to leave their positions by 2025. And experts at the Association of American Medical Colleges (AAMC) shared a similar estimation, saying that the US will come up short on physicians within just a dozen years, by somewhere between 37,800 and 124,000 doctors.
By one calculation, that is the number of US physicians in direct care who left the workforce between the start of 2019 and the fall of 2021, even before the Omicron wave slammed intensive care units and left too many doctors feeling desperate amid a "pandemic of mistrust," AAMC said on May 4.

A COVID-19 patient is brought into an emergency department in the Manhattan borough of New York City, US, on January 11, 2022. Photo: IC
A different strategy
American healthcare workers have been facing tremendous stress because the overall anti-epidemic strategy in the US is a mitigation policy, rather than an elimination policy, to curb the peak of the transmission, but the hospitalization rate for the past two years remained high, Chen Xi, an associated professor of public health at Yale University, told the Global Times.
"Although the hospitalization rates have recently dropped, the overall rates over the past two years remain very high, which means the medical staff have been working under stress and have been exposed to the risk of getting infected, which is why many of them have left their positions," Chen said.
In the initial phases of the COVID-19 pandemic, many US hospitals could not provide an adequate supply of beds to meet the demand, and the burgeoning Omicron variant is already overwhelming US hospitals because of high rates of hospitalization, Washington DC-based healthcare publication Health Affairs said in an article in February. When compared globally, the US has relatively low number of hospital beds, with only 2.8 beds per thousand people compared to 8.0 beds per thousand people in Germany, according to the publication.
According to the Chinese health authorities, China's number of hospital beds per thousand people increased from 6.30 in 2019 to 6.46 in 2020, but this is still behind some developed countries and regions.
Liang Wannian, head of the COVID-19 response expert panel under the National Health Commission (NHC), told a press conference on April 29 that as China has an unbalanced regional spread of population and a lack of medical resources in some areas, a strategy of "coexisting with the virus" would put too much pressure on the country's medical resources, posing a serious threat to those with underlying diseases, elderly groups, children and pregnant women.
Chinese health authorities, in accordance with the country's dynamic zero-COVID strategy, recently updated the COVID-19 treatment playbook to reduce the burden on Chinese medical workers. For example, mild cases are isolated rather than being taken to hospital, which can avoid hospitals becoming overwhelmed.
As the virus variant continues spreading in the US, the hospitalization rate will increase, highlighting the shortage of medical staff, Chen noted.
"In the next phase, the medical workers in the US will still be under a lot of stress," he said.



